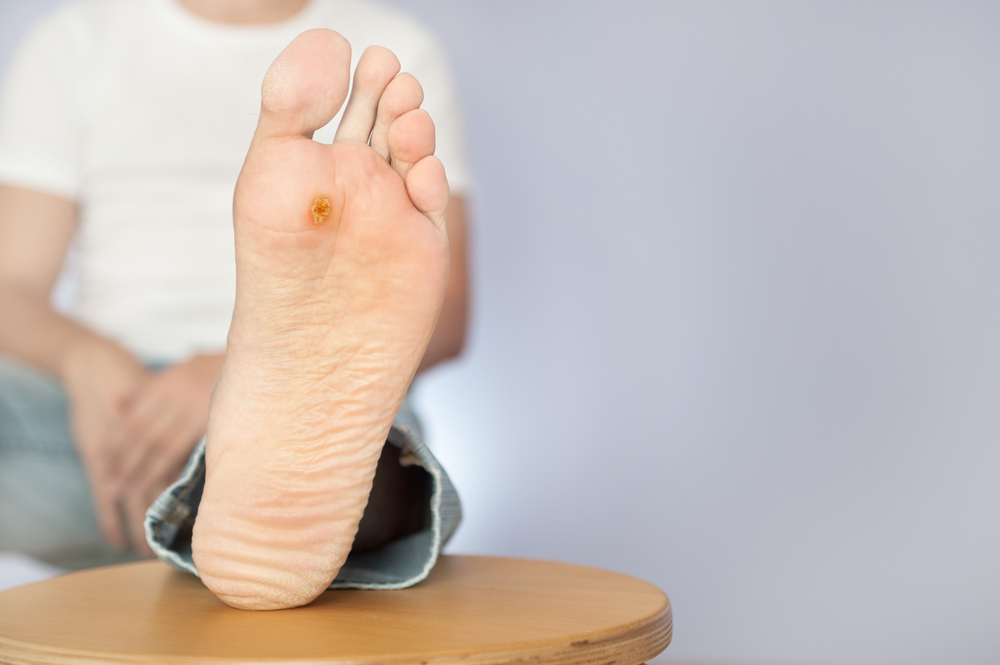
non-diabetic foot ulcer requires medical attention
A non-diabetic foot ulcer is an open wound or sore on the foot that occurs in people who do not have diabetes. While foot ulcers are commonly associated with diabetes, they can also develop due to a variety of other health conditions and external factors. What makes these ulcers concerning is that they can worsen quickly if not properly treated, leading to infection, delayed healing, and in severe cases, long-term complications.
Understanding why a non-diabetic foot ulcer requires medical attention is important to help prevent serious outcomes and support early recovery.
What Is A Non-Diabetic Foot Ulcer?
A non-diabetic foot ulcer is essentially a break in the skin on the foot that fails to heal properly. Unlike minor cuts or scrapes, these ulcers go deeper into the skin layers and sometimes affect underlying tissues.
They can appear on the heel, sole, toes, or side of the foot. In many cases, they begin as small injuries that worsen over time due to poor circulation, repeated pressure, or infection. Because the feet bear the body’s weight, even small wounds in this area are more likely to become serious if not managed correctly.
Common Causes Of Non-Diabetic Foot Ulcers
Non-diabetic foot ulcers can develop for several reasons, often related to poor blood flow, pressure, or trauma to the skin.
One of the most common causes is poor circulation, which reduces the body’s ability to deliver oxygen and nutrients needed for healing. Conditions such as peripheral artery disease (PAD) can significantly increase the risk.
Repeated pressure or friction is another major cause, especially in people who wear ill-fitting shoes or spend long hours standing. Over time, constant pressure can damage the skin and underlying tissue.
Infections can also contribute to ulcer formation, especially when small cuts or blisters are left untreated. Additionally, conditions such as venous insufficiency, autoimmune disorders, or physical injuries can increase the risk of developing foot ulcers.
Early Signs And Symptoms
Recognizing early signs of a non-diabetic foot ulcer is essential for preventing complications. In the beginning, the affected area may appear red, swollen, or irritated. The skin may feel warm to the touch and may be painful when pressure is applied.
As the condition progresses, an open sore may develop. This wound may not heal within a few days and may begin to deepen. In some cases, there may be drainage, an unpleasant odor, or signs of infection such as increased redness and swelling.
Because these symptoms can worsen gradually, many people delay seeking medical care until the ulcer becomes more severe.
Why Non-Diabetic Foot Ulcers Can Be Serious
Although these ulcers occur in people without diabetes, they can still become serious if ignored. One of the main concerns is infection. Once bacteria enter the wound, they can spread quickly to surrounding tissues and even into the bloodstream in severe cases.
Another concern is delayed healing. When blood flow is poor or pressure continues on the affected area, the body struggles to repair the damaged tissue. This can cause the ulcer to persist for weeks or even months.
In advanced cases, untreated ulcers can lead to deeper tissue damage, including muscle or bone involvement. This increases the risk of complications and may require more intensive medical treatment.
This is why seeking non-diabetic foot ulcer medical attention early is extremely important.
Who Is At Risk?
While anyone can develop a non-diabetic foot ulcer, certain individuals are more at risk. Older adults are more likely to experience poor circulation, which slows healing. People with vascular diseases such as peripheral artery disease are also at higher risk.
Individuals who have reduced mobility or spend long periods standing or sitting may develop pressure-related ulcers. Wearing tight or poorly fitted footwear can also increase the likelihood of skin breakdown.
Additionally, individuals with a history of foot injuries or chronic skin conditions may be more vulnerable.
How Non-Diabetic Foot Ulcers Are Diagnosed
Diagnosis usually begins with a physical examination of the affected area. A healthcare provider will assess the size, depth, and appearance of the ulcer. They may also check for signs of infection.
In some cases, additional tests are performed to understand the underlying cause. These may include blood tests to check for infection or inflammation, imaging tests such as X-rays to determine if deeper structures are affected, and vascular studies to evaluate blood flow in the legs and feet.
Accurate diagnosis is essential for creating an effective treatment plan.
Treatment Options For Non-Diabetic Foot Ulcers
Treatment depends on the severity and underlying cause of the ulcer. The main goals are to promote healing, prevent infection, and address any contributing health issues.
Wound Care
Proper wound care is essential. This may include cleaning the wound regularly, removing dead tissue (debridement), and applying specialized dressings to protect the area and promote healing.
Infection Control
If an infection is present, antibiotics may be prescribed. In more severe cases, stronger or intravenous antibiotics may be required.
Pressure Relief
Reducing pressure on the affected area is critical. Patients may be advised to wear special footwear, use cushioning devices, or limit weight-bearing activities to allow healing.
Improving Blood Flow
If poor circulation is a contributing factor, treatments may focus on improving blood flow. This can include medications, lifestyle changes, or procedures to restore proper circulation.
When To Seek Medical Attention
A non-diabetic foot ulcer should never be ignored. Medical attention is necessary if the wound does not begin to heal within a few days, becomes larger, or shows signs of infection such as redness, swelling, pus, or foul odor.
Severe pain, blackened tissue, or fever are also warning signs that require immediate medical care.
Early intervention can prevent complications and significantly improve healing outcomes.
Importance Of Early Treatment
Early treatment of a non-diabetic foot ulcer can prevent serious complications such as deep tissue infection or long-term mobility issues. When addressed quickly, most ulcers can heal effectively with proper wound care and management.
Delaying treatment increases the risk of chronic wounds, which are more difficult to treat and may require advanced medical interventions.
Clinical Research And New Treatment Options
Medical research continues to improve the way chronic wounds and foot ulcers are treated. Clinical trials play an important role in developing new therapies that enhance healing and reduce complications.
If you are interested in advanced treatment options or research participation, you can explore opportunities related to foot ulcers.
Final Thoughts
A non-diabetic foot ulcer may start as a small wound, but it can become a serious medical condition if not treated properly. Understanding the importance of non-diabetic foot ulcer medical attention is key to preventing complications and promoting healing.
With early diagnosis, proper wound care, and attention to underlying health conditions, most foot ulcers can be successfully managed. However, ignoring symptoms can lead to infection, delayed healing, and more severe outcomes.
If you notice any persistent foot wounds, seek NRA Clinical Diabetic Foot ulcer clinical trials in your area for the safest choice.